Lesson 4: Specific Preterm Infant Nutritional Management
4.2 Clinical and nutritional management in NEC
Treatment and management of NEC depends on the clinical status of the patient. Medical or surgical management may be required based on clinical manifestations (Neu & Walker 2011). Severe and advanced cases of NEC and those with bowel perforation will require surgical intervention (Table 8).
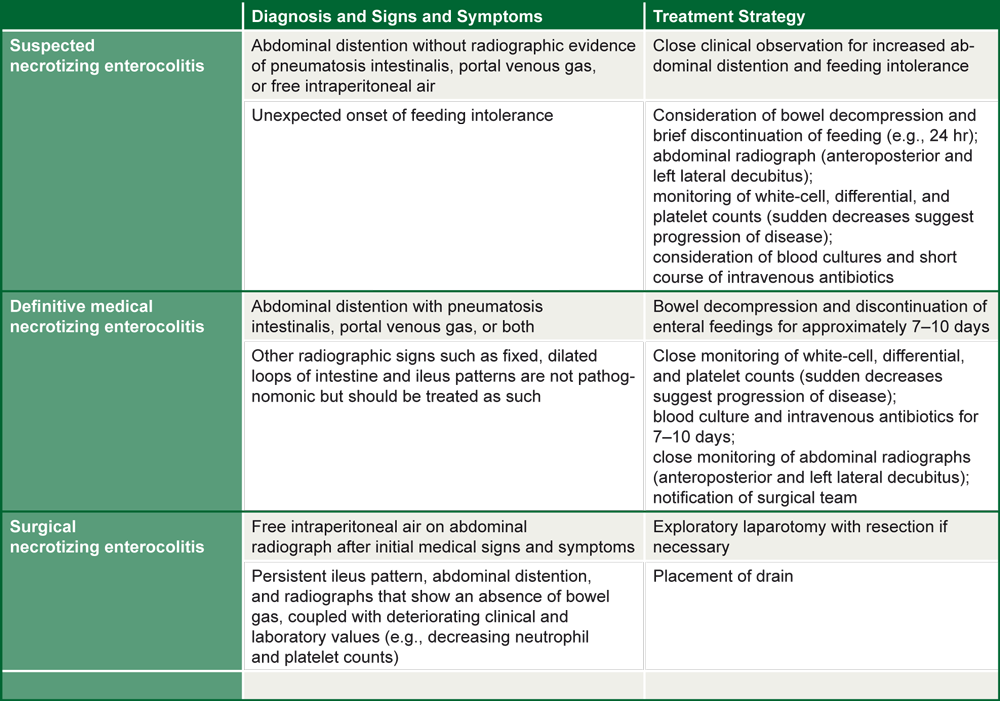
Table 8: Diagnostic Criteria for and Treatment of Necrotizing Enterocolitis
Source: Neu & Walker 2011
Medical management should start promptly, as soon as NEC is suspected. These include, nutritional management including withholding of enteral feeding, medical supportive care, antibiotic therapy and close monitoring (clinical, laboratorial and image - Fig 4) (Neu 2014):
First of all, all enteral feeding should be ceased.
- Gastrointestinal decompression, done by a large lumen gastric tube with either constant suction or intermittent aspiration.
- Total parenteral nutrition must be started with enough protein administration (3.5-4.0 g/kg/day), maintaining positive nitrogen balance and fuel for tissue reparation. The use of lipid emulsions is recommended for adequate energy intake. Lipids intake at approximately 3g/kg/day.
- Hemodynamic support with inotropes when necessary.
- Frequent laboratory monitoring of urine output, serum electrolytes and hematocrit.
- Blood cultures
- Initiation of empiric broad-spectrum antibiotics.
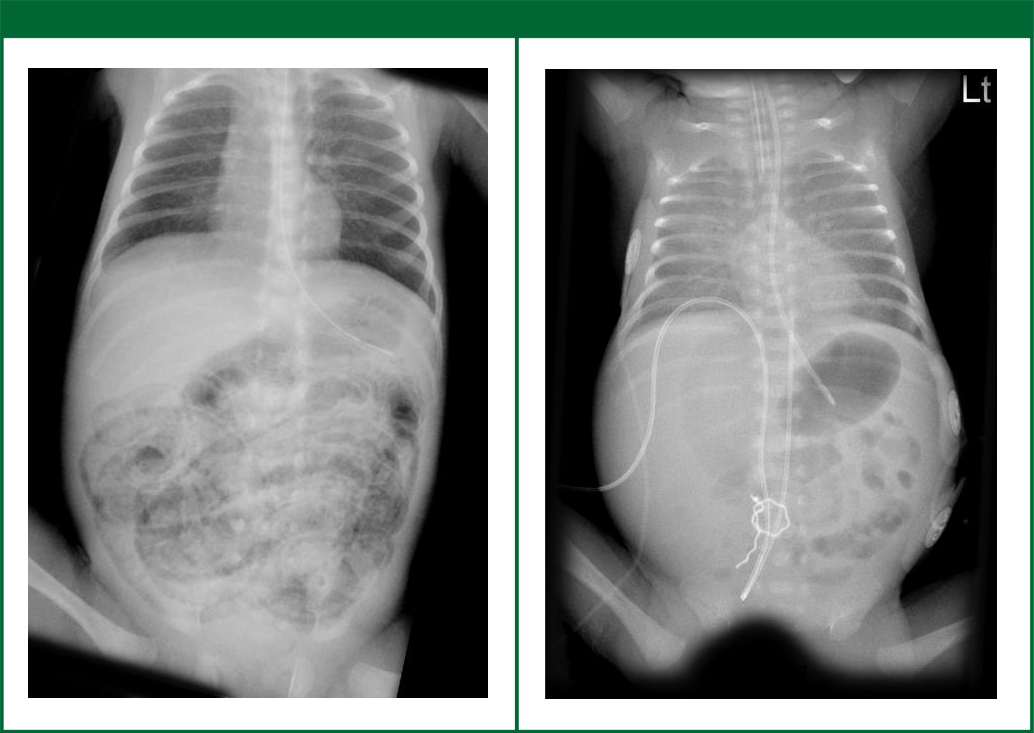
Surgical intervention may be necessary when there is important systemic deterioration even with proper clinical care. The other indication for surgical treatment is the presence of pneumoperitoneum (Figure 4) in radiological image due to bowel perforation.
Figure 4: Left - pneumatosis intestinalis (intramural gas); Right- pneumoperitoneum
Source: Case courtesy of Dr Frank Gaillard, from the case Necrotizing enterocolitis
Case courtesy of Dr Frank Gaillard, From the case Free peritoneal gas
Prevention
Early NEC recognition and aggressive treatment has improved the prognosis of preterm infants with the condition. However, NEC still represents with a substantial long-term morbidity for preterm infants, mainly those VLBW and ELBW. Therefore, preventive measures are very important in the NICU.
Several interventions have been studied for NEC prevention. Please refer to table 9.
Table 9. Prevention of NEC
Source: Neu 2014; reprinted with permission of S. Karger AG, Switzerland
Human milk is by far the best preventive measure against NEC. As already discussed in Unit 1 - Lesson 2.6, providing human milk to premature infants significantly decreases their risk of developing NEC. Donor's human milk may provide similar benefit, but further investigation is still warranted (Neu 2014).
Prediction
Prediction of infants with higher NEC risk is an important tool for prevention and management of NEC in the preterm infant. Prediction methods that have been developed and are non-invasive and include: profiling of fecal microbiome, oral swab collection from buccal epithelium for identification of inflammatory proteins (Neu 2014).