Lesson 5: Preterm Infant Nutritional Management in Low-resource Settings
5.1 Introduction and general principles
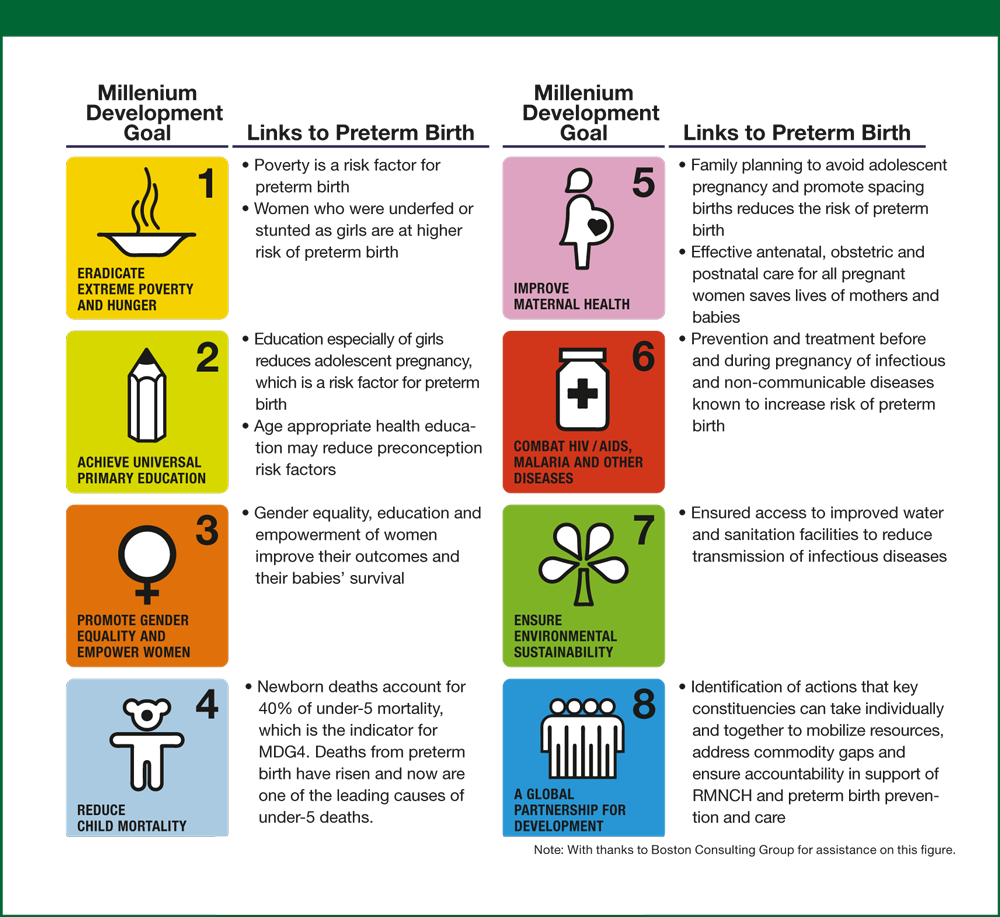
In developing countries, over 90% of infants born before 28 weeks will die, whereas in high income countries over 90% of these infants will survive. The World Health Organization (WHO) global action report "Born Too Soon,” published in 2012, outlines a public health approach to preterm birth (WHO et al. 2012). The Millennium Development Goals (MDG) launched in 2000 was established by 189 member states. MDG 4 and MDG 5 call for drastic reductions of maternal and infant mortalities by the end of 2015. The link between the MDGs and the prevention and care of preterm births is summarized in figure 6.
To combat the morbidity and mortality from preterm birth in developing countries, the first step is to focus on improvements in preconception and prenatal care such as birth control and treatment of maternal malnutrition. Implementing affordable perinatal interventions will also reduce morbidity and mortality - such as the use of antenatal steroids in case of preterm labor and antibiotics in mothers with premature rupture of membranes or in preterm infants at risk for sepsis. Promotion and support of breastfeeding is critical, as is the teaching of kangaroo mother care.
Figure 6. How the Millennium Development Goals link to prevention and care of preterm births.
Source: WHO et al. 2012
Nutritional management for the preterm infant actually starts in the womb. Interventions in low-resource countries to avoid maternal malnutrition should be started before conception. These intervention programs aim to diagnose and treat malnutrition in women at reproducible age. Many micronutrients (including vitamins and minerals) are deficient among women in low-resource countries, and nutrient deficits during pregnancy are linked with many adverse outcomes in the neonate. Low birth weight, congenital malformations, cretinism and even adult-onset chronic diseases have been described as consequences of maternal malnutrition (Murguia-Peniche & Kirsten 2014).
The use of antenatal corticosteroids in preterm birth is routine in most hospitals in high- and middle-income countries. A Cochrane review including 21 randomized trials (3885 women and 4269 infants) concluded that the use of antenatal corticosteroids was associated with a reduction of 31% in neonatal death (Roberts & Dalziel 2006). Based on these results, the WHO and other international agencies released reports encouraging the use of antenatal corticosteroids for women at risk of preterm birth in low-resource settings (WHO et al. 2012). Only 5 to 10% of the women in low- income countries receive such treatment (Murguia-Peniche & Kirsten 2014). However, a new study by Althabe and colleagues (Althabe et al. 2015) has revealed that the scale-up of antenatal corticosteroids treatment in low-resource countries, as planned by the WHO, may actually be harmful. The study, an international cluster randomized trial including almost 100 000 pregnant women in six low and middle-income countries, reported an increase of 12% in overall newborn mortality, 11% increase in perinatal mortality and 45% increase in the risk of suspected maternal infection in the corticosteroid treatment intervention group. There was no effect on the survival of preterm or small infants. The trial investigators concluded their report urging caution in deployment of antenatal corticosteroids treatment in low-resource countries (Althabe et al. 2015).
During the neonatal period an important intervention in low-resource countries is the practice of delayed cord clamping (DCC). Already discussed in Unit 2 Lesson 7, DCC has been shown to increase placental transfusion and consequently increases neonatal blood volume at birth by 30% (Garofalo & Abenhaim 2012). In preterm infants, a recent meta-analysis has shown that DCC reduces the need for transfusions and the risks for intraventricular hemorrhage and NEC. Therefore, DCC in low-resource settings represents a valuable tool when blood banks and safe transfusion practices are not available (Murguia-Peniche & Kirsten 2014).
Management of the preterm infant, especially VLBW and ELBW infants, is still challenging everywhere in the world. However, in low-resource countries this challenge can be even more daunting. Innovation might be the solution in these low-resource settings, and in the next part of this lesson we will describe the innovative approach from a group dealing with communities with a very low socioeconomic status in the Tygerberg Children's Hospital from the University of Stellenbosch in Cape Town, South Africa.
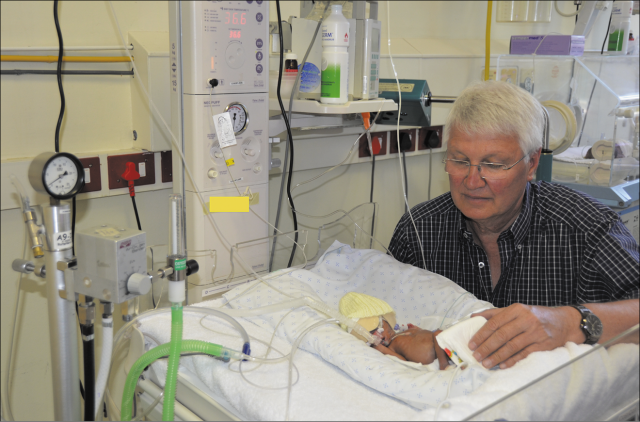
Professor Gert Kirsten, Head Neonatal Division in Tygerberg Children's Hospital and a preterm infant in the Neonatal ward.
Source: reprinted with kind permission of Gert Kirsten